First MTP arthrodesis (big toe fusion) relieves severe foot pain by permanently locking the arthritic joint to stop painful grinding. Find the right surgeon who fits your needs below, serving Canadians in major cities like Vancouver, British Columbia; Edmonton, Alberta; Toronto, Ontario; and Montréal, Québec.
The information on this website is intended for informational purposes only and is not a substitute for medical, legal, or financial advice. Always consult a health provider, legal counsel, or financial professional if you have questions or concerns. The use of the information on this website does not create a physician-patient relationship between Surgency and you.
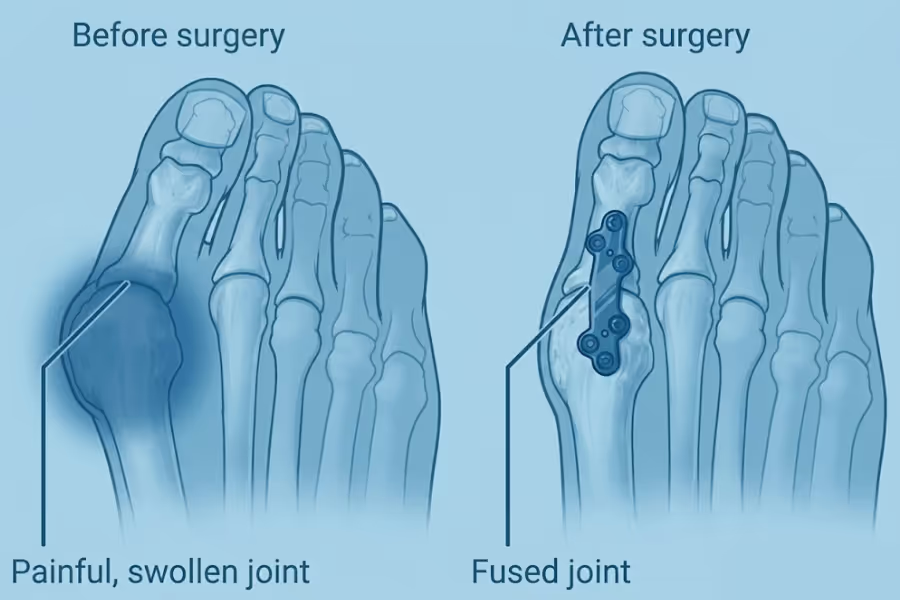
First MTP arthrodesis (often called a big toe fusion) is a surgery for the foot that relieves severe pain caused by arthritis or extreme bunions. It works by removing the damaged cartilage and permanently joining the two bones of the big toe joint (the metatarsophalangeal joint) together into one solid bone.
Think of the big toe joint like a door hinge that must bend every time you push off to take a step. When severe arthritis (a condition called hallux rigidus) wears away the smooth cartilage, the bones grind directly against each other. This creates massive bone spurs, severe stiffness, and sharp pain every time you walk.
Why do it? When clinical exams and X-rays confirm severe, bone-on-bone arthritis and every step hurts, a fusion permanently stops the grinding. While the toe will no longer bend at that specific knuckle, the pain relief is usually excellent. Most people walk much better after surgery than they did before because the sharp arthritis pain is completely gone.
Public waitlists for orthopaedic foot and ankle consults, X-rays, and OR time can be long—especially because toe arthritis is often not considered a medical emergency. Private centres can sometimes line up assessment and surgery in weeks rather than months, cutting time spent limping, avoiding walks, and squeezing into painful shoes.
Going private can let you:
You know who’s operating, when it’s happening, and what hardware they’ll use. Predictable dates make it easier to arrange time off work and prepare for the required resting and recovery period.
Private pathways may offer streamlined imaging, advanced surgical hardware, and coordinated anaesthesia/pain/physiotherapy plans—with virtual follow‑ups if you live far away.
Typical first MTP arthrodesis surgery takes about 1 to 1.5 hours of operating time. Add time at the centre for check‑in, anaesthesia, and recovery (usually a few extra hours).
You meet the team, confirm the correct foot, review imaging, and go over the plan. Safety checks are done (including marking the correct toe).
Usually general anaesthesia (you’re fully asleep) or twilight sedation. The anaesthesiologist or surgeon will often perform a regional "nerve block" (freezing the foot/ankle) to ensure you wake up with very little pain.
You’re positioned comfortably on your back. The foot and leg are cleaned and draped sterilely. A tourniquet is often used on the calf to minimize bleeding.
An incision (usually 2 to 3 inches long) is made on the top or side of the big toe joint. The surgeon gently moves tissues aside to reach the bones.
The surgeon removes the massive bone spurs and completely strips away the remaining damaged cartilage to prepare the bone ends for fusion.
The toe is placed in the perfect position for walking. The surgeon then secures the two bones together using small titanium screws, and often places a small metal plate across the top of the joint for extra stability.
The surgeon uses a live X-ray machine (fluoroscopy) to confirm the hardware is perfectly placed and the toe angle is exact.
Layers are closed with sutures (stitches). The foot is heavily bandaged and placed in a specialized rigid post-op shoe or a surgical boot.
You recover in the post‑anaesthesia care unit, begin gentle movement when safe, and receive wound‑care instructions. Almost all patients go home the same day.
Every foot is different—follow your surgeon’s plan. A fusion requires the bones to physically knit together, which takes time.
Reality check:
Foot throbbing, swelling, and a feeling of heaviness are extremely common. The nerve block will wear off in the first 24 to 48 hours, causing a temporary spike in pain.
Goals: Control pain, keep swelling down, and protect the hardware.
Activities: Elevation is your full-time job. Keep your foot elevated above your heart as much as possible. You will wear a stiff surgical shoe or boot. Depending on your surgeon, you may be allowed to walk strictly on your heel (heel-bearing only) or you may need to use crutches/a knee scooter to keep all weight off the foot. Keep the bandages completely dry.
Still annoying but improving.
Goals: Wound healing, transition to more mobility, avoid flare‑ups.
Activities: You will have your first follow-up to check the incision and remove stitches. You will likely continue wearing the stiff post-op shoe to protect the toe. You can gradually spend more time on your feet, but swelling will still occur if you stand too long.
The work phase.
Goals: Confirm bone healing and transition to normal footwear.
Activities: You will get new X-rays around the 6-week mark to check if the bones have fused. Once cleared by your surgeon, you can usually transition out of the surgical shoe into a stiff-soled, roomy running shoe (like a Hoka). You will slowly return to light household tasks and longer walks.
Confidence building.
Goals: Near‑normal daily activity; walking without a limp.
Activities: Progress your walking distances. The bone is usually solidly fused by this point. You can return to most low-impact activities like cycling or swimming.
Back to most normal life.
Goals: Return to usual routines, hiking, and heavier activities.
Activities: You can add impact and heavier activity with clearance. Note: Foot swelling after a long day can persist for up to 6 months to a year. This is normal.
Exact prices depend on the surgical facility, the specific titanium hardware used (plates and screws), and whether any other toes need to be fixed at the same time. Always ask for a written, itemized quote.
Typical range: $8,000 - $14,000+
Typical range: CA$12,000 - CA$25,000+
Ask if it’s a global bundle and request line items for: surgeon, facility, anaesthesia, implants (hardware cost), imaging, follow‑ups, and what triggers extra charges (e.g., if additional time is needed to fix a severe deformity).
Choosing your surgeon is a major benefit of pursuing private surgery. Here’s how to choose wisely for a first MTP arthrodesis (big toe fusion).
Ask how many big toe fusions they perform each year.
A big toe fusion is highly “precision-dependent” because:
Also ask about their case mix:
For a more in-depth guide read, How to Understand Surgeon Credentials in Canada
Request recent data, ideally for foot fusions specifically:
Make sure they confirm you’re a good candidate for a fusion, not just a cleanup procedure.
A careful surgeon should explicitly assess:
Ask:
Good programs use imaging to confirm candidacy:
Choose accredited centres (e.g., Accreditation Canada / CAAASF) with:
You want a written plan for:
Request an itemized quote including:
Clarify add-ons:
Surgeon and plan
Technique and safety
Recovery and after-care
Costs and logistics
First MTP arthrodesis (big toe fusion) is a specific solution for end-stage arthritis (hallux rigidus) or massive joint deformity. It is right for patients who need to eliminate severe, daily pain and are willing to trade the bending motion of the joint for a pain-free, stable foot.
Most private surgical clinics in Canada require a referral from a family doctor, walk-in clinic physician, or specialist. Your referring doctor will send over your medical records, imaging, biopsy results, and relevant blood work.
If you don't have a family doctor, many private clinics can help you navigate the referral process or connect you with a physician who can provide one, so you can still reach out, even if you don't have a referral.
Your surgeon’s instructions come first—follow their plan if it differs.
Prepare your upper body and "good" leg
Quit nicotine
Medication review
Safe layout
Mobility aids and elevation
Bath setup
Clothing
Meal prep
Constipation plan
Skin prep
What to bring
Your personal risk depends on your bone quality, anatomy, and general health. Discuss your specific risks with your surgeon.
Your situation depends on how bad your daily pain is, whether you can still walk comfortably, and how fast the arthritis is progressing.
Severe joint destruction
Compensatory pain (Kinetic chain issues)
Loss of mobility and fitness
Medication dependence
If you still have questions, please feel free to contact us directly.
Please note: Surgency is not a clinic itself. Nor can we help with emergency situations, or provide personalized medical advice—that is between you and your surgeon. If you are experiencing acute or severe symptoms, please present to your local emergency department or urgent care centre.


Board-certified foot and ankle surgeon specializing in minimally invasive forefoot reconstruction and diabetic limb salvage–trained reconstructive foot and ankle surgery, with 8 years of experience.


Triple-fellowship-trained orthopedic surgeon dedicated to getting active patients back on their feet. Specializing in foot and ankle reconstruction, sports injuries, and minimally invasive surgical techniques.


Highly experienced orthopedic surgeon with over 30 years of experience. Regarded as a regional leader in foot and ankle surgery, focused on complex deformities, sports injuries, degenerative conditions.