Biceps tenodesis relieves chronic shoulder and upper arm pain by detaching the damaged long head biceps tendon from the shoulder and reattaching it to the upper arm bone (humerus). Find the right shoulder surgeon who fits your needs below, serving Canadians in major cities like Vancouver, British Columbia; Edmonton, Alberta; Toronto, Ontario; and Montréal, Québec.

The information on this website is intended for informational purposes only and is not a substitute for medical, legal, or financial advice. Always consult a health provider, legal counsel, or financial professional if you have questions or concerns. The use of the information on this website does not create a physician-patient relationship between Surgency and you.
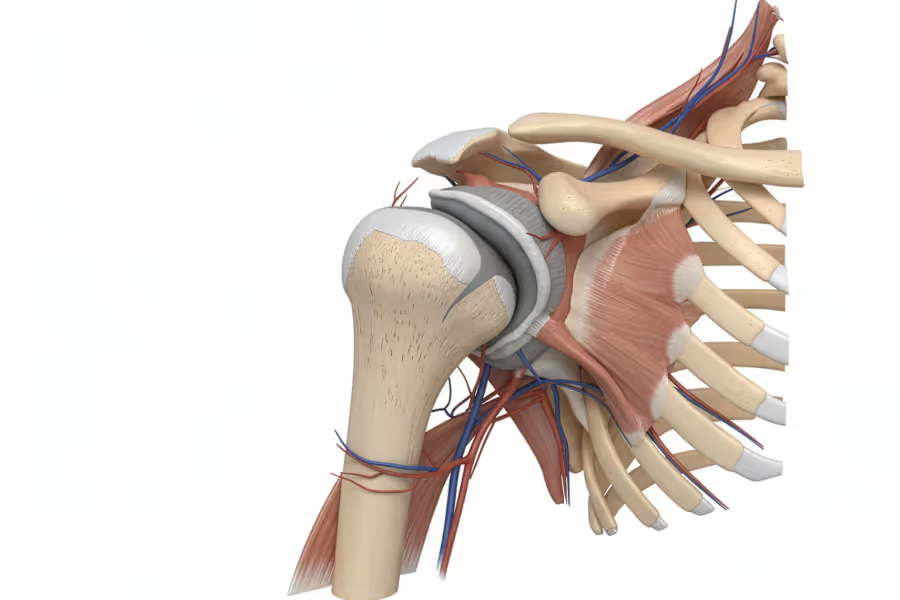
Biceps tenodesis is a surgery for the shoulder that treats pain and dysfunction caused by damage to the long head of the biceps tendon (LHBT)—the tendon that connects the top of your biceps muscle to the shoulder socket (specifically, the labrum and the top of the glenoid).
Think of the long head biceps tendon like a rope anchored to the top of your shoulder socket. Over time—or after an injury—that rope can fray, partially tear, become inflamed (tendonitis), or slip out of its groove (subluxation). When this happens, you get pain in the front of the shoulder, aching down the upper arm, and weakness with lifting or overhead movements. The biceps tendon is also commonly involved when the labrum tears at the top of the socket (a SLAP tear).
Biceps tenodesis can be performed arthroscopically (through small keyhole incisions with a camera), as a mini-open procedure (small incision near the front of the shoulder or upper arm), or as a subpectoral open procedure (incision in the armpit crease). Your surgeon will choose the technique based on where the tendon damage is and what other shoulder work is needed.
Why do it? When shoulder pain from biceps tendon damage persists despite rest, physio, and injections—especially if it's affecting sleep, work, sport, or daily activities—biceps tenodesis offers a reliable way to eliminate the pain source while preserving the muscle's strength and appearance.
Shoulder surgery often faces lengthy queues for consultation, imaging (MRI), and OR time. Instead of waiting months, private centres can schedule surgery within weeks—reducing time spent with front-of-shoulder pain, night pain, and activity restrictions, and helping you return to work, sport, or daily life sooner.
Going private can let you:
You know who's operating, when it's happening, and the detailed plan (fixation technique, concomitant procedures, rehab milestones). Clear timelines reduce anxiety and help families and employers coordinate support.
Private pathways may offer streamlined imaging, coordinated surgical and rehab plans, and virtual follow-ups if you live far away.
Biceps tenodesis typically takes about 45–90 minutes of operating time when performed as an isolated procedure. When combined with other shoulder work (rotator cuff repair, labral debridement, subacromial decompression), total time may be 1.5–2.5 hours. Expect a few extra hours at the centre for check-in, anaesthesia, and recovery before heading home. This is almost always a same-day (outpatient) procedure.
1. Check-in and marking
You meet the team, the surgeon marks the shoulder, and you review the plan.
2. Anaesthesia
You'll get general anaesthesia (asleep) and often a nerve block (interscalene block) to numb the shoulder and arm for pain control after surgery.
3. Position and prep
You're positioned safely (beach-chair or lateral). The skin is cleaned and covered with sterile drapes.
4. Diagnostic look (arthroscopy)
The surgeon inserts a small camera through keyhole incisions to inspect the shoulder joint—confirming the biceps tendon damage and checking the rotator cuff, labrum, and cartilage.
5. Biceps tendon release
The damaged tendon is cut from its attachment at the top of the shoulder socket (labrum).
6. Tenodesis (reattachment)
The tendon is pulled to its new position on the humerus. A small hole or socket is prepared in the bone, and the tendon is secured with an interference screw, suture anchor, or button fixation device. The surgeon sets the correct tension so the biceps muscle functions normally.
7. Additional work (if needed)
If there's a rotator cuff tear, labral damage, bone spurs, or impingement, these are addressed in the same session.
8. Close up
Small incisions are closed with stitches or strips, covered with a dressing, and a sling is fitted.
9. Wake-up and instructions
You recover in the post-anaesthesia care unit, get discharge instructions for the sling and early movement, and head home the same day.
Every shoulder is different—follow your surgeon's plan. Taking rehab seriously usually means better results. Some private clinics offer virtual follow-ups or coordinate physio near home.
Reality check: Soreness, swelling, stiffness, and tough sleep. Not fun. The nerve block may keep the arm numb for a day.
Goals: Control pain and swelling, protect the repair, start safe motion.
Activities: Wear the sling as directed (typically 3–4 weeks). Ice and elevate. Keep the incision clean and dry. Move fingers, wrist, and elbow. Gentle pendulum exercises if cleared by your surgeon. A helper is useful for dressing, meals, and medication.
Still annoying but improving.
Goals: Gradually restore pain-free range of motion (ROM) within limits; stay safe in the sling.
Activities: Regular physio begins. Passive to assisted ROM (forward elevation and external rotation to set limits). Scapular setting exercises. Light daily tasks at waist level. No active biceps curling, no resisted elbow flexion, and no forearm supination against resistance for at least 6 weeks—this protects the healing tenodesis.
The work phase.
Goals: Wean from sling (as cleared). Near-full ROM by ~8 weeks. Begin gentle strengthening.
Activities: Start gentle active ROM. Initiate resisted biceps curls and supination only when cleared (usually around 6 weeks). Rotator cuff and scapular strengthening with light resistance bands. Posture work. Controlled functional use below shoulder height.
Building strength and confidence.
Goals: Full ROM, better strength and endurance, stable shoulder with everyday use.
Activities: Progress resistance exercises (biceps, rotator cuff, deltoid, scapula). Closed-chain work (wall/plank variations). Coordination and sport-prep drills (no contact or heavy overhead yet). Low-impact cardio as cleared.
Return to full activity.
Goals: Power, endurance, and trust in the shoulder.
Activities: Sport-specific and work-specific drills. Gradual return to overhead work, heavy lifting, and contact sports only when cleared by your surgeon and physio. Full recovery typically takes 4–6 months.
Exact prices depend on whether biceps tenodesis is performed as an isolated procedure or combined with rotator cuff repair, labral work, or subacromial decompression, and where you have it done. Combined procedures cost more. Always ask for a written, itemized quote.
Typical range: $8,000 - $20,000+
Note: Costs increase when tenodesis is combined with rotator cuff repair or other shoulder procedures. Some centres offer bundled pricing.
Typical range: CA$12,000 - $35,000+
Varies widely by setting (ambulatory surgery centre vs. hospital), state, and whether additional procedures are performed.
Ask if it's a global bundle and request line items for: surgeon, facility, anaesthesia, implants/hardware, nerve block, imaging review, sling, and follow-ups, and what triggers extra charges (e.g. if rotator cuff repair or labral work is added once the surgeon is in the joint).
Choosing your surgeon is one of the biggest benefits of going private—use it to your advantage.
Ask how many biceps tenodesis procedures they perform per year, and their case mix:
Higher volume and routine outpatient pathways usually correlate with smoother care and fewer complications.
For a more in-depth guide read, How to Understand Surgeon Credentials in Canada
Request recent data:
A careful surgeon should:
Ask:
Confirm the clinic is accredited (e.g. Accreditation Canada / CAAASF) with shoulder-appropriate equipment, experienced anaesthesia, and trained staff.
A written, phased rehab protocol with clear timelines for:
Request an itemized quote including:
Clarify what triggers additional charges (e.g. adding rotator cuff repair, extra anchors, longer OR time).
Surgeon and plan
Technique and safety
Recovery and aftercare
Costs and logistics
Biceps tenodesis is specifically designed to eliminate pain from the long head biceps tendon while preserving the muscle's strength and appearance.
Most private surgical clinics in Canada require a referral from a family doctor, walk-in clinic physician, or specialist. Your referring doctor will send over your medical records, imaging, biopsy results, and relevant blood work.
If you don't have a family doctor, many private clinics can help you navigate the referral process or connect you with a physician who can provide one, so you can still reach out, even if you don't have a referral.
Your surgeon's instructions come first—follow their plan if it differs.
Shoulder "prehab"
Quit nicotine
Medication review
Safe layout
Clothing
Sleep setup
Food and supplies
Surgency is free for patients, funded for by surgeons.
Surgeons—who meet our listing criteria—pay a flat fee to list on the Surgency platform. To maintain objectivity, there are no commissions, referral fees, nor any ranking or recommending one surgeon over another. Surgency is patient-first. Our goal is to make the process of finding a private surgeon as simple as possible. You choose who to contact. Learn more in our Advertising Policy.
Your personal risk depends on the extent of surgery (isolated tenodesis vs. combined with rotator cuff repair), fixation technique, and your general health. Discuss your specific risks with your surgeon.
Your situation depends on symptom severity, the degree of tendon damage, your activity level, and whether other shoulder structures are involved.
If you still have questions, please feel free to contact us directly.
Please note: Surgency is not a clinic itself. Nor can we help with emergency situations, or provide personalized medical advice—that is between you and your surgeon. If you are experiencing acute or severe symptoms, please present to your local emergency department or urgent care centre.


Triple-fellowship orthopedic surgeon specializing in elbow and shoulder procedures who treats professional athletes and active individuals looking to return to sport safely and quickly.