Cervical laminectomy & discectomy relieve pressure on the spinal cord and nerves in the neck by removing bone and herniated disc material. Find the right surgeon who fits your needs below, serving Canadians in major cities like Vancouver, British Columbia; Edmonton, Alberta; Toronto, Ontario; and Montréal, Québec.
À titre informatif seulement, ne constitue pas un avis médical ou juridique. Veuillez consulter votre médecin ou votre chirurgien.
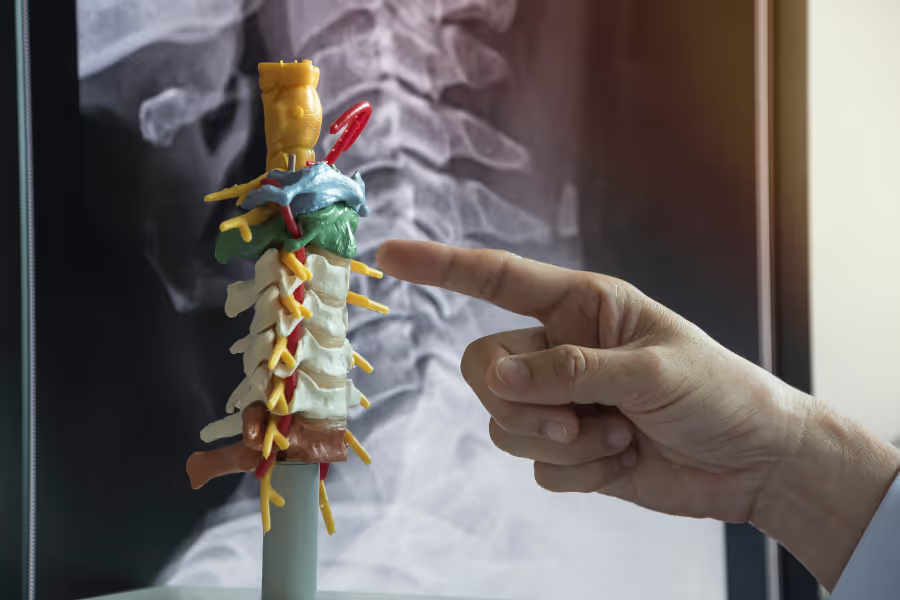
Cervical laminectomy and discectomy are surgeries for the neck (cervical spine) that relieve pressure on pinched nerve roots and/or the spinal cord. Think of the spinal canal like a hallway. In the neck, extra bone from arthritis (bone spurs), thickened ligaments, or a herniated cervical disc can crowd that hallway, squeezing nerves and sometimes the spinal cord—leading to arm pain, numbness/tingling, weakness, clumsiness, balance problems, or (in more severe cases) symptoms of spinal cord compression.
A laminectomy widens the hallway. The surgeon removes part of the lamina—the bony “roof” over the spinal canal—to create more space around the spinal cord and nerves. A discectomy targets the disc itself. The surgeon removes the portion of the herniated disc that has bulged out and is compressing a nerve root or the spinal cord. Many patients have both steps in the same operation: make space (laminectomy) and remove the disc fragment (discectomy). The surgeon may also use a microscope or minimally invasive tools depending on the level and anatomy.
Why do it? When imaging (like an MRI) matches your symptoms—such as cervical radiculopathy from a herniated disc or cervical stenosis from bone overgrowth—surgically clearing the pressure can let the nerve and/or spinal cord “breathe,” improving pain and function and helping prevent worsening neurologic deficits. The goal is simple: decompress the nerve/spinal cord so symptoms improve and you can move more confidently.
Public wait lists for spine consults, MRI, and OR time can be long—especially if your symptoms are severe but not considered emergent. Private centres can sometimes line up assessment and surgery in weeks rather than months, cutting time spent with arm pain, numbness/weakness, sleep‑killing pain, or (in some cases) progressing spinal cord symptoms like clumsiness or balance trouble.
Passer au privé peut vous permettre de :
You know who’s operating, when it’s happening, and the approach they’ll use. Direct communication and predictable dates make it easier to arrange time off, travel, and post‑op physiotherapy.
Private pathways may offer:

Typical single‑level cervical decompression often takes about 1.5 - 3 hours of operating time, depending on approach and complexity. Add time at the centre for check‑in, anaesthesia, and recovery (usually a few extra hours). Multi‑level, revision, or complex stenosis cases can take longer.
1. Enregistrement et confirmation
You meet the team, confirm the cervical level(s), review imaging, and go over the plan. The surgical site is marked and safety checks are done (including side/level verification).
2. Anesthésie
General anaesthesia (you’re fully asleep). Many centres use X‑ray guidance; some use neuromonitoring depending on cord/nerve risk and surgeon preference.
3. Poste et préparation
You’re positioned carefully (often on your back for anterior approaches or on your stomach for posterior approaches). The neck area is cleaned and draped sterilely.
4. Petite incision et exposition
A short incision is made. The surgeon gently moves tissues aside to reach the spine while protecting nearby structures.
5. Laminectomy (make space)
From a posterior approach, the surgeon removes part of the lamina (the “roof” of the spinal canal) and may trim thickened ligament/bone spurs to widen the canal and relieve pressure.
6. Discectomy (remove the culprit)
If a disc herniation is compressing a nerve root or the cord, the surgeon removes the offending disc fragment. Bone spurs may also be smoothed if they’re contributing to narrowing.
7. Rincez et vérifiez
The area is irrigated. The surgeon confirms decompression and may verify levels with X‑ray.
8. Gros plan
Layers are closed with sutures; a dressing is applied. A drain is sometimes used, depending on the approach and extent.
9. Réveil et instructions
You recover in post-anesthesia care unit, begin gentle movement when safe, and receive wound‑care and activity instructions. Many patients go home the same day; some stay overnight based on complexity, pain control, and medical history.
Chaque cou est différent — suivez le plan de votre chirurgien. Un progrès constant et intelligent vaut mieux que de pousser trop fort.
Reality check: neck soreness, tight muscles/spasms, low energy, and some swallowing discomfort can occur (especially with anterior approaches). Arm symptoms may improve quickly, but numbness can take longer.
Goals: control pain, protect the neck, walk safely.
Activities: short, frequent walks; gentle shoulder/arm movement as allowed; keep the incision clean/dry. Avoid heavy lifting and sudden neck movements. If given a collar/brace, wear it exactly as prescribed.
Still annoying but improving.
Goals: build a walking habit, reduce stiffness, avoid flare‑ups.
Activities: daily walks increasing time/distance; light self‑care at counter height; start prescribed physio if/when cleared. Many people return to desk/school work (often with restrictions). Stitches removed if needed.
The work phase.
Goals: better posture, endurance, and controlled strength without stressing the neck.
Activities: longer walks; upright stationary bike if cleared; gentle upper‑back/scapular strengthening; gradual return to light household tasks. Continue to avoid heavy lifting and high‑impact activity unless specifically cleared.
Confidence building.
Goals: near‑normal daily activity; gradual fitness.
Activities: progress strengthening and mobility with guidance. Many people are significantly improved by this point, though nerve recovery can continue.
Back to most normal life (for many).
Goals: return to usual routines; work/sport‑specific training if approved.
Activities: add impact and heavier lifting only with explicit clearance. Keep neck‑smart habits (neutral posture, avoid prolonged awkward positions).
Exact prices depend on how many levels are treated (one vs. two or more); whether you need a laminectomy, discectomy, or both; overall complexity (primary vs. revision surgery); and where you have it done. Hospital stays, advanced imaging, and special tech (navigation/neuromonitoring) can push costs higher. Always ask for a written, itemized quote.
Typical range: $21,000 - $40,000+
Typical range: $32,000 - $100,000+
Ask if it’s a global bundle and request line items for: surgeon, facility, anaesthesia, implants/supplies, imaging, neuromonitoring, navigation, follow‑ups, and what triggers extra charges (e.g., adding another level).
Choosing your surgeon is a major benefit of pursuing private surgery. Here’s how to choose wisely for cervical spine procedures.
Ask how many cervical laminectomies/discectomies they perform yearly.
Request recent data:
Make sure non-operative care was considered (physio, medications, injections) unless there is urgent cord compression. Clear reasons for surgery = better expectations.
Surgery is usually not the first step if the issue is mild neck pain or a new pinched nerve that is improving with time. It is something you consider when the nerve or spinal cord compression is chronic, worsening, or refuses to respond to non-surgical care. Mechanical compression (bone spurs or large disc fragments) rarely disappears on its own.
No, you do not need a referral for a private cervical laminectomy & discectomy in Canada. You can book a consultation directly with a surgeon, and they will review your options and diagnostics.
Les instructions de votre chirurgien sont prioritaires — suivez son plan s'il diffère.
Smoking/vaping slows healing and raises infection risk. Stopping 4+ weeks before surgery (and staying off afterward) helps.
Préparation des repas
Plan contre la constipation
Pain plan
Jeûne
Préparation de la peau
Your personal risk depends on your health, the level(s) involved, the exact problem (soft disc herniation vs. bone-spur stenosis), whether the spinal cord is compressed, the approach/technique (microsurgical, minimally invasive, anterior vs posterior), anaesthesia, and how closely you follow post‑op instructions. Discuss your specific risks with your spine surgeon.
Your situation depends on symptom severity, what imaging shows (disc herniation vs stenosis, which level and side), whether there are signs of spinal cord compression (myelopathy), your daily demands (work/school/sport), and how well non‑surgical care is working. Talk specifics with your spine surgeon.
Progressive pain and functional limits
Worsening nerve problems (radiculopathy)
Spinal cord progression (if myelopathy is present or developing)
Mechanics and anatomy can worsen
Diminution de la qualité de vie et déconditionnement
Inconvénients liés aux médicaments
Si vous avez encore des questions, n'hésitez pas à nous contacter directement.


Neurochirurgien ayant grandi dans la région, spécialisé en neurochirurgie à accès minimal et en neurochirurgie endovasculaire; avec un intérêt clinique pour la neurochirurgie cérébrovasculaire, spinale et oncologique, et 21 ans d'expérience.


Un neurochirurgien de grande renommée, reconnu pour la chirurgie mini-invasive de la colonne vertébrale, spécialisé dans les soins complets du cerveau, du cou et du dos, et comptant 8 ans d'expérience.


Un chef de file en reconstruction spinale complexe, chef de la chirurgie de la colonne vertébrale à Hamilton Health Sciences, reconnu pour son expertise en techniques mini-invasives et dans la gestion des déformations rachidiennes et de l'oncologie.