Turbinate reduction (including advanced techniques like turbinate coblation) improves nasal airflow by gently shrinking the swollen tissues inside your nose. Find the right surgeon who fits your needs below, serving Canadians in major cities like Vancouver, British Columbia; Edmonton, Alberta; Toronto, Ontario; and Montréal, Québec.
The information on this website is intended for informational purposes only and is not a substitute for medical, legal, or financial advice. Always consult a health provider, legal counsel, or financial professional if you have questions or concerns. The use of the information on this website does not create a physician-patient relationship between Surgency and you.
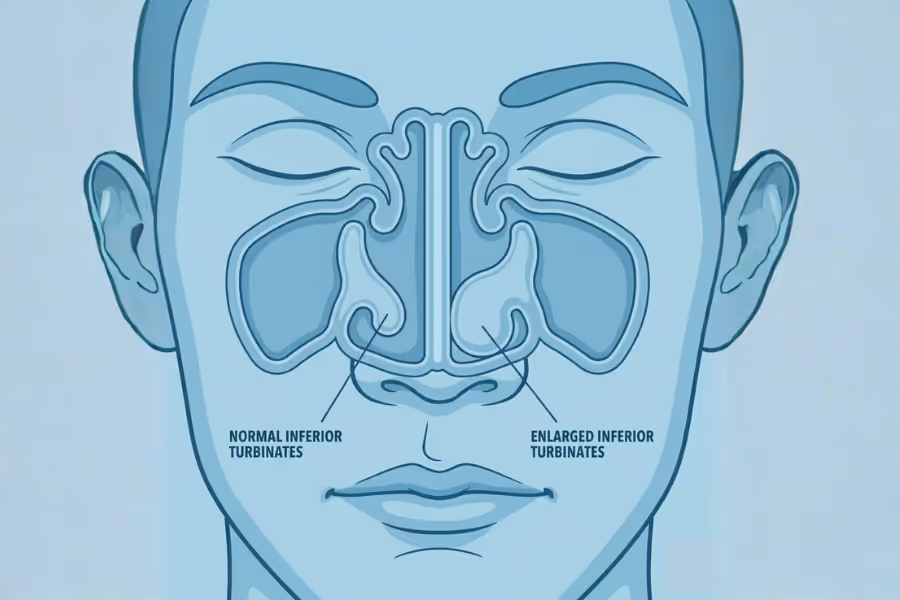
Turbinate reduction is a procedure for the nose that improves breathing by shrinking the inferior turbinates—soft, fleshy ridges along the sidewalls of your nasal cavity that warm, filter, and humidify the air you breathe.
Think of your turbinates like the air filters in a car. They are highly sensitive and do an important job. However, if they become chronically irritated by allergies, dust, or non-allergic rhinitis, they swell up like balloons. When these "filters" get too big, they block the nasal passage. This causes chronic congestion, mouth breathing, snoring, poor sleep, and an inability to use a CPAP machine for sleep apnea.
What actually happens
Surgeons use several methods to shrink the tissue while carefully preserving the outer lining (mucosa) so your nose doesn't become too dry.
Why do it? When months of steroid nasal sprays and allergy pills fail to shrink the swelling, turbinate reduction physically opens the airway. This allows you to breathe comfortably through your nose, improving your sleep, exercise stamina, and overall quality of life.
Public waitlists for an ENT (Ear, Nose, and Throat) consult and operating room time can take over a year—especially because nasal congestion is rarely considered a medical emergency. Private centres can often line up an assessment and surgery in weeks rather than months, cutting time spent struggling to sleep, breathing through your mouth, and relying on temporary nasal sprays.
Going private can let you:
You know exactly who is operating and what technology they will use. Predictable dates make it easier to arrange a few days off work while you manage the initial post-op congestion.
Private pathways offer streamlined imaging (like CT scans), advanced surgical tools (like coblation wands), and thorough follow-up care to ensure your nose heals correctly without excessive crusting or scarring.
Typical turbinate reduction (including coblation cases) often takes about 20–60 minutes of operating time. Add time at the centre for check‑in, anaesthesia, and recovery (usually a few extra hours). Combined procedures (like septoplasty) take longer.
You meet the team, review symptoms, confirm the plan (turbinate reduction ± septoplasty), and complete safety checks.
Depending on your clinic and complexity:
You lie on your back. The nose is numbed and prepared. Medications may be used to reduce bleeding.
The surgeon works through the nostrils using a small camera (endoscope). No external cuts.
If coblation is used, the surgeon inserts the coblation wand into or along the turbinate tissue and applies controlled energy to shrink it. The lining is preserved as much as possible.
The surgeon may also perform an outfracture to increase space further.
Bleeding is controlled. Some surgeons use:
You wake up in the recovery area, get written instructions (saline rinses, activity limits), and go home the same day.

Every nose is different—follow your surgeon’s plan. Many people expect instant relief, but congestion often gets worse briefly due to swelling.
Reality check: Congestion, crusting, and blood‑tinged mucus are common. Mild nosebleeds can happen.
Goals: Reduce swelling, prevent bleeding, and keep the nose clean.
Activities: Rest, short walks, sleep with your head elevated. Use saline sprays/rinses as directed. Avoid heavy lifting, hot yoga/saunas, bending over, and nose blowing (often for 1 week).
Still annoying but improving.
Goals: Less crusting and steadier airflow.
Activities: Continue saline rinses. Some clinics perform a gentle in‑office clean‑out (debridement) if crusts are significant. Many people are back to normal school/desk work quickly.
The work phase.
Goals: Stable nasal breathing, fewer flare‑ups.
Activities: Gradual return to full exercise if cleared. Continue allergy control if allergies are a driver—surgery creates space, but allergens can still cause swelling.
Most healing is complete and the final breathing result is clearer.
Exact prices depend on whether it’s done in‑office vs in an operating room, what technique is used (coblation/radiofrequency vs surgical reduction), and whether it’s combined with septoplasty or sinus surgery. Always ask for a written, itemized quote.
Typical range: $3,000 - $9,000+
Note: Pricing is often higher if done under general anaesthesia or bundled with septoplasty.
Typical range: $4,000 - $10,000+
Ask if it’s a global bundle and request line items for: surgeon, facility, anaesthesia, technique/device costs (including coblation), follow‑ups, and what triggers extra charges (adding septoplasty, extra OR time).
Choosing your surgeon is a major benefit of pursuing private surgery. Here’s how to choose wisely for turbinate reduction and turbinate coblation.
Ask how often they perform nasal airway surgery, not just “general ENT.”
Good questions:
Nasal airway work can be “precision-dependent” because outcomes rely on:
For a more in-depth guide read, How to Understand Surgeon Credentials in Canada
Request recent data, ideally for turbinate reduction specifically:
Also ask how they define success:
Make sure they confirm you’re a good candidate—not just “able to pay for it.”
A careful surgeon should explicitly assess:
They should compare surgery to:
Ask:
High-quality programs usually include:
Confirm the findings match:
Choose accredited centres (e.g., Accreditation Canada or other recognized surgical facility standards) with:
You want a written plan for:
Request an itemized quote including:
Clarify add-ons:
Diagnosis and plan
Technique and safety
Recovery and after-care
Costs and logistics
Turbinate reduction (including coblation) is meant for people whose main problem is chronic nasal obstruction from enlarged turbinates that does not improve enough with appropriate medical therapy.
Most private surgical clinics in Canada require a referral from a family doctor, walk-in clinic physician, or specialist. Your referring doctor will send over your medical records, imaging, biopsy results, and relevant blood work.
Your surgeon’s instructions come first—follow their plan if it differs.
Optimize nasal health (before surgery)
Quit nicotine
Medication review
Safe layout
Sleep setup
Food and hydration
What to bring
Plan time off
Know the basic do’s and don’ts
Your personal risk depends on your anatomy, the technique used (including coblation), and your general health. Discuss your specific risks with your surgeon.
Your situation depends on how severe your blockage is and what’s causing it (turbinates vs septum vs valve vs polyps).
If you still have questions, please feel free to contact us directly.
Please note: Surgency is not a clinic itself. Nor can we help with emergency situations, or provide personalized medical advice—that is between you and your surgeon. If you are experiencing acute or severe symptoms, please present to your local emergency department or urgent care centre.


A global authority in sleep surgery with 18 years of experience, specializing on nasal and sinus complaints, rhinoplasty, orbit and tear duct surgery, endoscopic sinus surgery, snoring and sleep apnea.