Eustachian tube balloon dilation relieves chronic ear pressure, fullness, and muffled hearing by gently widening a blocked Eustachian tube from inside the nose. Find the right surgeon who fits your needs below, serving Canadians in major cities like Vancouver, British Columbia; Edmonton, Alberta; Toronto, Ontario; and Montréal, Québec.
The information on this website is intended for informational purposes only and is not a substitute for medical, legal, or financial advice. Always consult a health provider, legal counsel, or financial professional if you have questions or concerns. The use of the information on this website does not create a physician-patient relationship between Surgency and you.
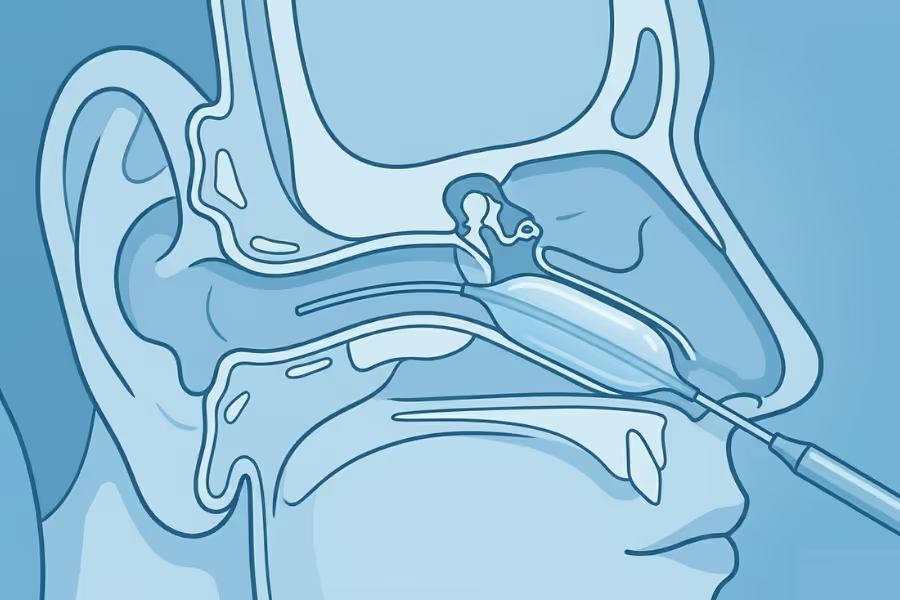
Eustachian tube balloon dilation (also called balloon tuboplasty or balloon Eustachian tuboplasty) is a minimally invasive surgery for the ear that relieves chronic blockage of the Eustachian tube—the narrow passage connecting the middle ear to the back of the nose—by inflating a small balloon catheter inside the tube to widen it and restore normal function.
Think of the Eustachian tube like a pressure-relief valve for your ear. Every time you swallow, yawn, or pop your ears, the tube opens briefly to equalize pressure between the middle ear and the outside world. When the tube stays swollen, inflamed, or blocked, pressure builds up behind the eardrum. This can cause ear fullness or a plugged sensation, muffled hearing, popping or crackling sounds, ear pain, dizziness, and in some cases recurrent middle ear infections or fluid buildup.
What actually happens
Why do it? When nasal sprays, decongestants, and other treatments haven't resolved your Eustachian tube dysfunction, balloon dilation can restore the tube's ability to equalize pressure—helping relieve that persistent plugged-ear feeling and improving hearing and comfort.
Eustachian tube balloon dilation is not routinely publicly funded or widely available in every part of Canada. In many cases, patients must pay out of pocket if they want this procedure done privately. Even where ENT assessment is publicly covered, the balloon device itself or access to a surgeon who offers the procedure may not be. This means you can see a private surgeon in your home province for this procedure.
Public ENT consults, hearing tests, and OR access can still take time—especially for conditions like chronic eustachian tube dysfunction that affect quality of life but are not considered emergencies. Private care can sometimes move from assessment to treatment in weeks rather than months.
Going private can let you:
You know who is performing the procedure, when it is happening, and what the treatment plan is. Predictable timing can make it easier to arrange time off, travel, and follow-up care.
Private pathways may offer streamlined hearing tests, nasal endoscopy, and coordinated follow-up plans, with virtual follow-ups if you live far away.
Typical Eustachian tube balloon dilation often takes about 15–30 minutes of procedure time per side. Add time at the centre for check-in, anaesthesia, and recovery (usually a few extra hours). Bilateral cases (both ears) take slightly longer.
1. Check-in and confirmation
You meet the team, confirm which side(s) will be treated, review imaging, and go over the plan. Safety checks are completed.
2. Anaesthesia
General anaesthesia (fully asleep) or local anaesthesia with sedation, depending on surgeon preference and patient factors. Many cases are done under general anaesthesia for comfort.
3. Position and prep
You're positioned on your back. The nasal passages are prepared with decongestant and anaesthetic.
4. Endoscopic access
A small endoscope (camera) is inserted through the nostril to visualize the opening of the Eustachian tube at the back of the nose. No external incisions are made.
5. Balloon catheter insertion
A thin balloon catheter is guided through the nose and into the Eustachian tube under direct visualization.
6. Balloon inflation
The balloon is inflated with saline to a controlled pressure for approximately two minutes, gently dilating the cartilaginous portion of the tube.
7. Deflation and removal
The balloon is deflated and carefully removed. If both sides are being treated, the process is repeated on the other side.
8. Final check
The surgeon confirms the tube opening looks adequate and checks for any bleeding.
9. Wake-up and instructions
You recover in the post-anaesthesia care unit, and receive wound-care and activity instructions. Most patients go home the same day.
Every ear is different—follow your surgeon's plan. This is one of the quicker recoveries in surgical medicine.
Reality check:
Mild nasal congestion, minor ear fullness, and low energy from anaesthesia are common. Some patients notice immediate improvement; others find it takes a couple of weeks for the full benefit. Minor nosebleeds or blood-tinged mucus are normal.
Goals: Rest, stay hydrated, and avoid anything that creates pressure in the nose or ears.
Activities: Light activity around the house. Avoid blowing your nose (or blow very gently if absolutely necessary). No heavy lifting, straining, or bending over. Sneeze with your mouth open.
Improving steadily.
Goals: Gentle return to normal routine; protect the healing tube.
Activities: Most people return to desk or school work within 2–3 days. Continue avoiding forceful nose blowing. Nasal saline rinses as directed by your surgeon. Light walking is fine.
The settling phase.
Goals: The Eustachian tube remodels and function improves.
Activities: First post-op review (usually around 2–3 weeks). Your surgeon will assess improvement in your ability to equalize your ears. Resume gentle exercise if cleared. Most daily activities are unrestricted by this point.
Full assessment.
Goals: Confirm sustained improvement.
Activities: Second post-op review. A symptom questionnaire (ETDQ-7) may be repeated to objectively measure change. Return to full activity including flying, diving, and exercise as cleared.
Exact prices depend on whether one or both sides are treated, the balloon system used, and where you have it done. Eustachian tube balloon dilation is not covered by most provincial health insurance plans (e.g., OHIP in Ontario) as it is considered a newer procedure. Always ask for a written, itemized quote.
Cost in Canada (private)
Typical range: $4,500 - $8,000+
Note: Bilateral (both sides) is typically at the higher end. Costs may be higher if combined with other procedures such as septoplasty or sinus surgery.
Cost in the United States
Typical range: CA$6,000 - CA$13,000+
What's usually included
What's often not included
Tips to compare quotes
Ask if it's a global bundle and request line items for: surgeon, facility, anaesthesia, balloon catheter device, endoscopy, follow-ups, and what triggers extra charges (e.g., bilateral treatment, combination with sinus surgery).
Choosing your surgeon is a major benefit of pursuing private surgery. Here's how to choose wisely for Eustachian tube balloon dilation.
Experience and volume (balloon dilation–specific)
Ask how many Eustachian tube balloon dilations they perform each year (not just general ENT procedures).
Balloon dilation requires familiarity with Eustachian tube anatomy and proper patient selection because:
Also ask about their case mix:
Credentials and training
For a more in-depth guide read, How to Understand Surgeon Credentials in Canada
Outcomes and safety (ask for real numbers)
Request recent data, ideally for balloon dilation specifically:
Clear indications and alternatives
Make sure they confirm you're a good candidate for balloon dilation, not just "able to pay for it." Note: This shouldn't be a problem, as Canadian surgeons are bound to act in the patient's best interests.
A careful surgeon should explicitly assess:
They should also compare balloon dilation to:
Surgical plan
Ask:
Imaging and planning (must be thorough)
Good programs use imaging and testing to confirm candidacy:
Confirm the findings match your specific ear symptoms and side (left vs. right vs. both).
Facility accreditation and safety systems
Choose accredited centres (e.g., Accreditation Canada / CAAASF) with:
Rehab integration
You want clear instructions for:
Transparent pricing
Request an itemized quote including:
Clarify add-ons:
Surgeon and plan
Technique and safety
Recovery and after-care
Costs and logistics
Signals of a high-quality balloon dilation program
Eustachian tube balloon dilation is right for patients with obstructive Eustachian tube dysfunction who haven't improved with conservative treatment and want a minimally invasive, tissue-preserving option.
Most private surgical clinics in Canada require a referral from a family doctor, walk-in clinic physician, or specialist. Your referring doctor will send over your medical records, imaging, biopsy results, and relevant blood work.
If you don't have a family doctor, many private clinics can help you navigate the referral process or connect you with a physician who can provide one, so you can still reach out, even if you don't have a referral.
Your surgeon's instructions come first—follow their plan if it differs.
Manage allergies and nasal inflammation
Quit nicotine
Medication review
Light cardio
Stock up on supplies
Safe layout
Eating and fasting
Skin/nasal prep
What to bring
Practice ahead
Red flags to know
Your personal risk depends on your anatomy, whether one or both sides are treated, and your general health. Discuss your specific risks with your surgeon.
Your situation depends on symptom severity, how long you've had Eustachian tube dysfunction, and whether complications like middle ear fluid or eardrum retraction are developing.
Chronic middle ear fluid (effusion)
Eardrum retraction and damage
Recurrent ear infections
Progressive hearing loss
Quality of life
Medication dependence
When watchful waiting can be reasonable
When not to delay (seek prompt assessment)
If you still have questions, please feel free to contact us directly.
Please note: Surgency is not a clinic itself. Nor can we help with emergency situations, or provide personalized medical advice—that is between you and your surgeon. If you are experiencing acute or severe symptoms, please present to your local emergency department or urgent care centre.


A global authority in sleep surgery with 18 years of experience, specializing on nasal and sinus complaints, rhinoplasty, orbit and tear duct surgery, endoscopic sinus surgery, snoring and sleep apnea.