
The information on this website is intended for informational purposes only and is not a substitute for medical, legal, or financial advice. Always consult a health provider, legal counsel, or financial professional if you have questions or concerns. The use of the information on this website does not create a physician-patient relationship between Surgency and you.
Surgency is a free resource for Canadian patients and caregivers. Private pathways Canadian physician in the public system to help you find the right surgeon for your needs.

As a family doctor in the public system, I believe transparency is a form of care. I created Surgency to help my patients struggling on long waitlists who wanted to understand all their options for timely medical attention.
Surgency is a free resource designed to empower and educate—helping you understand private pathways and find accredited surgeons within Canada. I hope Surgency brings you clarity.
Dr. Sean Haffey

Pilonidal cyst excision is a surgical procedure that removes a chronic cyst, infection, or sinus tract located at the tailbone (the top of the buttocks/gluteal cleft).
A pilonidal cyst is often more than just a simple lump. It is usually a nest of hair and debris that has burrowed under the skin, creating a sinus tract (tunnel) that leads to the surface. Unlike a general body-wide sinus tract or an anal fistula (which connects to the bowel), a pilonidal sinus is confined to the skin and fat of the tailbone area but is notorious for being recurrent and difficult to heal due to friction and hair growth.
In an excision, the surgeon aims to remove the entire cyst cavity, the skin pores (“pits”) that allow hair to enter, and the chronically inflamed tract lining. Depending on the size, infection history, and complexity, the surgeon may:
This surgery is different from simply treating flare-ups with antibiotics or incision and drainage (I&D). Those steps can relieve acute pain and release pus during an infection, but they do not remove the hair nest or the tract—so the problem usually keeps recurring.
Time matters when pilonidal disease keeps flaring—painful abscesses, persistent drainage, odour, ruined clothing, and repeated antibiotics or urgent care visits. Private clinics can often book assessment and treatment sooner, reducing months of “bandage management” and missed work/school/gym.
You know who will do the procedure, what technique is planned (open healing vs. closure vs. flap), what aftercare looks like (dressings, drains, hair control), and when follow-ups happen. A clear date and itemized quote make planning time off easier.
Pilonidal surgery is often an outpatient procedure. Procedure time commonly ranges 30–90+ minutes, depending on how extensive the sinus tracts are and whether a flap/cleft‑lift is done. Expect to be at the clinic or surgical centre for several hours including intake and recovery.
1) Check-in and confirmation
2) Anaesthesia
3) Prep and sterile setup
4) Excision and tract management
5) Closure (or open healing)
6) Same-day discharge
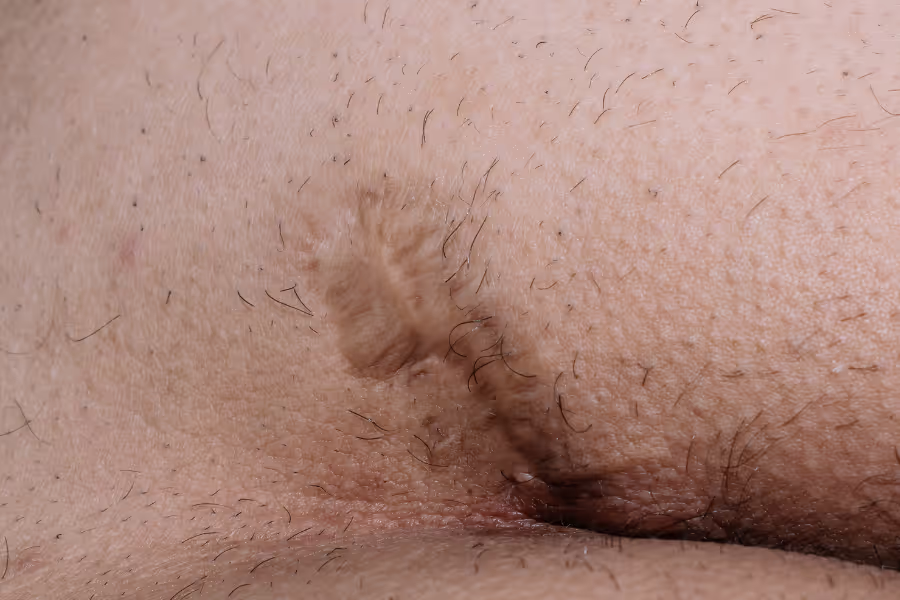
Your surgeon’s instructions come first. Recovery depends heavily on the technique (open healing vs. closed/flap) and how extensive the disease is.
What it feels like
Main goals
Typical instructions
What it feels like
Main goals
Typical steps
What it feels like
Main goals
Typical steps
Pilonidal surgery is usually more expensive than a simple skin cyst excision because it often involves deeper tissue, a higher infection/recurrence risk, and (commonly) sedation or general anesthesia in an accredited surgical centre rather than a basic procedure room.
Typical range for private surgery in Canada: $2,500 - $6,500+
Limited disease / simpler excision ($2,500 - $3,500)
Chronic or recurrent disease with off‑midline closure ($3,500 - $5,500)
Complex/recurrent/extensive disease ($5,500 - $6,500+)
Medically necessary pilonidal care can be covered publicly, but private excision is out-of-pocket. Some extended health plans may reimburse limited portions—ask the clinic for an itemized invoice.
Choosing your surgeon is one of the benefits of going private. Here’s how to choose wisely.
Pilonidal excision is usually not the first step if the issue is a one-time, small abscess that heals well. It is something you consider when the disease is chronic, recurrent, or refuses to heal. Pilonidal sinuses rarely disappear permanently without removing the pits and tracts.
Yes and no—you can reach out to any of the private surgeons listed on Surgency without a referral. Their intake teams are happy to answer questions, explain what they treat, share pricing ranges, and walk you through next steps.
However, to book a formal consultation with the surgeon, you'll typically need a referral from your family doctor or nurse practitioner. Don't have one? Many of the clinics can help coordinate a virtual GP appointment to get the referral paperwork sorted. All surgeons listed on Surgency offer virtual initial consultations, so you don't need to travel until you and the surgeon have agreed on a plan.
Before your consultation, expect the clinic to request relevant medical records and recent diagnostic imaging (X-ray, MRI, CT, ultrasound, lab work, etc.). Having these ready speeds up the process and lets the surgeon give you specific guidance on your very first call.
Your surgeon will give you a specific plan. Preparation focuses on hygiene and reducing infection risk in this bacteria-prone area.
Surgency is free for patients, funded for by surgeons.
Surgeons—who meet our listing criteria—pay a flat fee to list on the Surgency platform. To maintain objectivity, there are no commissions, referral fees, nor any ranking or recommending one surgeon over another.
Surgency is patient-first. Our goal is to make the process of finding a private surgeon as simple as possible. You choose who to contact. Learn more in our Advertising Policy.
Your situation depends on how extensive your pilonidal disease is (single pit vs. multiple pits/sinus tracts), how often it flares, whether you’ve needed incision & drainage (I&D) before, and what your exam shows. Some cases can be managed for a while, but pilonidal disease often runs in cycles—and delay can mean more infection episodes and more complex disease. Review your personal risks with a clinician.
More flare-ups: swelling, pain, and drainage
Pilonidal disease commonly alternates between “quiet” and “active.” Delaying definitive treatment can mean more episodes of painful swelling, drainage, and downtime—often interfering with sitting, driving, work/school, exercise, and sleep.
Higher chance of abscess and infection (and urgent visits)
A blocked pilonidal sinus can form a tailbone abscess, which may require urgent I&D and antibiotics. Recurrent abscesses can mean repeated urgent care visits, repeated antibiotics (and side effects), and repeated missed days.
The disease can spread and become more complex over time
Ongoing inflammation can lead to:
More scarring and harder surgery later
Repeated infections and prior drainages create scar tissue that can:
Ongoing skin breakdown, odour, and constant wound care
Chronic drainage can irritate the surrounding skin, cause rashes and breakdown, stain clothing, and keep you stuck in daily pads/gauze and hygiene workarounds.
Impact on quality of life and mental load
Many people start avoiding long drives, desk work, cycling, gym, swimming, intimacy, or travel because they can’t trust the area not to flare or drain. The unpredictability (“Will it abscess again this week?”) is a real burden.
Rarely: missing something else
Most issues in this location are pilonidal, but if a wound is atypical, not in the usual cleft location, unusually firm, or not healing as expected, delaying assessment can delay diagnosis of other skin or soft-tissue problems.
Delaying excision may make sense if:
Every surgery has risks. Your personal risk depends on your overall health, the extent of disease, whether it’s inflamed/infected, the technique used (open healing vs. closed/off-midline closure), and how closely you follow wound-care instructions. Review your specific situation with your surgeon.
If you still have questions, then feel free to contact us directly.